Dr. Mark Madden, MD, FRCPC, Diagnostic and Interventional Radiologist Rapidly rolls out ultrasound to the patients amid COVID-19 restrictions (Ultrasound: ICU, CT Suite, Pre-Op)
Overview
Dr. Mark Madden is a diagnostic and interventional radiologist in a hospital that serves as a community tertiary referral center located in North Vancouver, Canada. The hospital has a few hundred beds and has a good-sized referral base. It provides a wide range of services including care for most specialties with few exceptions like cardiothoracic. Dr. Madden has a very busy active practice working in the radiology department and traveling to peripheral hospitals located along the coast and in nearby mountains where he provides onsite services as well as reaching out to remote sites via tele-radiology.
Challenge
The peripheral rural communities typically have smaller hospitals which may not have the same services as those offered at Dr. Madden's urban hospital. As a result, many transfers happened. It is a daily challenge to get the patients needing a higher level of care down from the rural areas and to the Vancouver hospital for their healthcare needs.
Some patients live in communities far away from equipment and modern staples of medical imaging and diagnosis. Dealing with the logistics of doing a procedure is challenging. “Sometimes the thing you’re actually trying to do is actually quite quick and easy. It’s just getting everyone together and making it work that is the challenge”, said Dr. Madden.
Then Covid Hit
In addition to the logistics of getting rural patients to the urban hospital for the services they needed, COVID introduced a new level of daily challenges within the hospital and radiology department. There were new workflows introduced to reach out to patients prior to their visit to determine if symptomatic, and when they arrived at the hospital the patients were further reviewed to determine if appropriate PPE was required. MOCK codes were introduced to deal with CPR and ACLS. Every single facet of what the radiologists did was affected.
Workflows had to change to adapt to COVID. Patients that might otherwise have been brought to the radiology department were now seen in the ICU. Dr. Madden explains:
“As an interventional radiologist, I frequently have to go to the ICU to perform a procedure on a patient. First, I have to unplug the heavy US machine, get the patient data, then unplug and move it down the hall, up an elevator, down the hall again and into ICU. It is very heavy, like hundreds of pounds. If it is rolled over your foot, it would probably break your toe. Once I get to the ICU, I have to plug in and wait for the software to re-boot.”
All of the ICU rooms were adapted for COVID. This takes up a lot of space in an already cramped space. There are large machines, with big footprints making it hard to navigate around all the tubing and IV poles. It is hard to perform a procedure when the radiologists are not comfortable in their ergonomics. They must squeeze into small spaces, compromise body mechanics, and pay the price with back problems at the end of the day. This is all exacerbated due to PPE like N95’s, googles, and doubled gloves & gowns, all of which can result in the radiologist becoming uncomfortable.
“Heavier machines don’t drive very smoothly and make it harder to avoid running over the cables that are connected to the patient. During COVID it was best to leave the patients in ICU rather than bring them to the radiology department. This way they maintain the needed ICU support and it avoids the risk of their lines being pulled out or compromised by traveling to the radiology department.”
So, how can the radiologist:
- quickly adapt to new workflows?
- quickly and easily move to the ICU and get close to the patient?
- avoid unnecessary safety risks associated with a large cart and dangling cables?
- perform timely and safe ultrasound procedures?
Solution
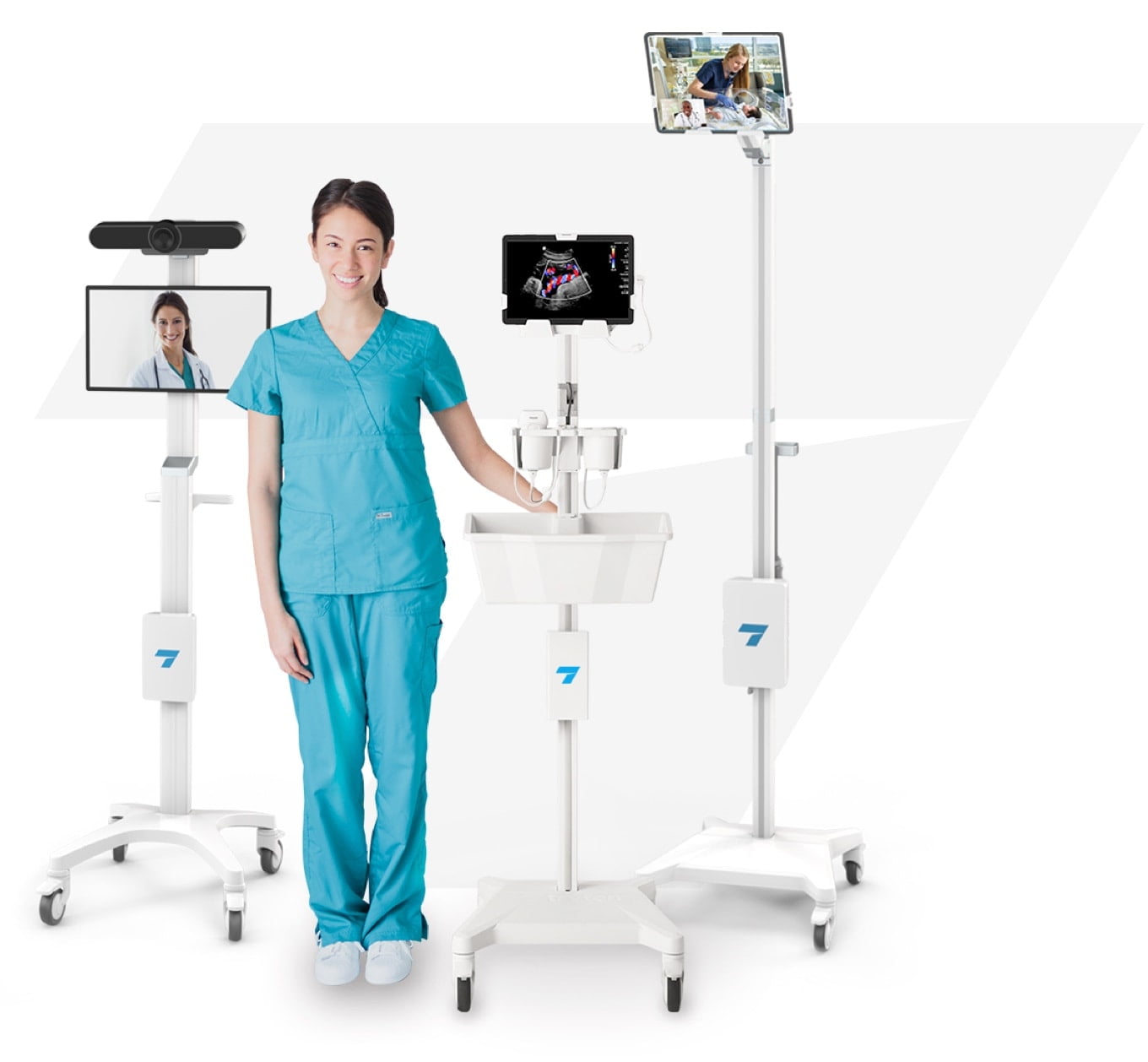
Dr. Madden realized he needed a portable, easy to position ultrasound with a small footprint that would allow him to quickly get to the ICU, set up in a very small space and quickly perform a procedure. The answer was a cart-based portable ultrasound with wireless transducers. Dr. Madden chose the Tryten S1 Tablet and Medical Device Cart because it is:
- lightweight, easy to position, and requires a small footprint
- designed for safe and secure cable management
- built for tablet-based ultrasound including storage for transducers and ultrasound gel.
The Benefit
Dr. Madden was able to rapidly adapt when COVID hit and now can quickly provide the interventional radiology services that are needed. He can quickly grab his Tryten S1 Tablet and Medical Device Cart, run to the ICU, position himself close to the patient, and perform a procedure without the concern of dangling cables, or the struggle of pushing and maneuvering hundreds of pounds worth of cart and ultrasound. The Tryten S1 cart is:
- Easier to quickly move to ICU and patients.
- Better able to quickly position cart and tablet screen for better viewing and ergonomics.
- Adaptable to different workflows so the radiologist can bring ultrasound to anywhere.
- Designed for an improved provider and patient experience.
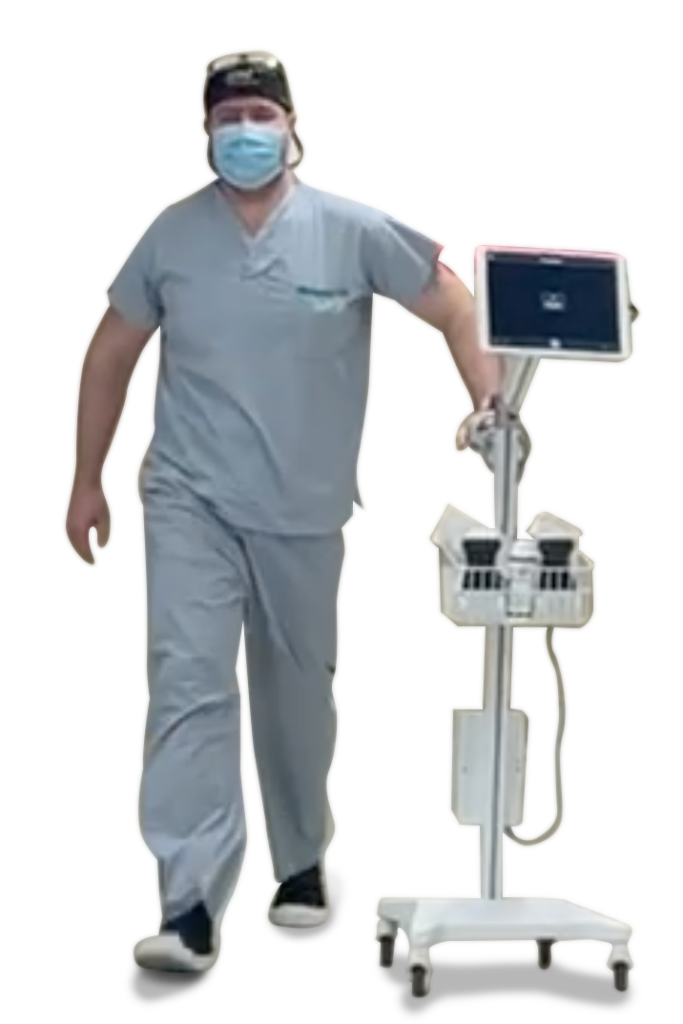
"It’s really helped us to have a much more portable solution
when we go up there something with a small footprint, stable, easy to see, easy to use…"
- Dr. Mark Madden, MD, FRCPC
Dr. Madden was able to pivot during Covid and continues to benefit from the agility and time saving
qualities of his solution.
Download a PDF of this Article here

Dr. Mark Madden, MD, FRCPC
Diagnostic and Interventional Radiologist
Born and raised in Vancouver BC, Canada. Completed medical school and Residency at UBC. Interventional Radiology fellowship at Auckland City Hospital in New Zealand. Huge fan of family, travel, electric cars and life in general!
Healthcare solutions for today!